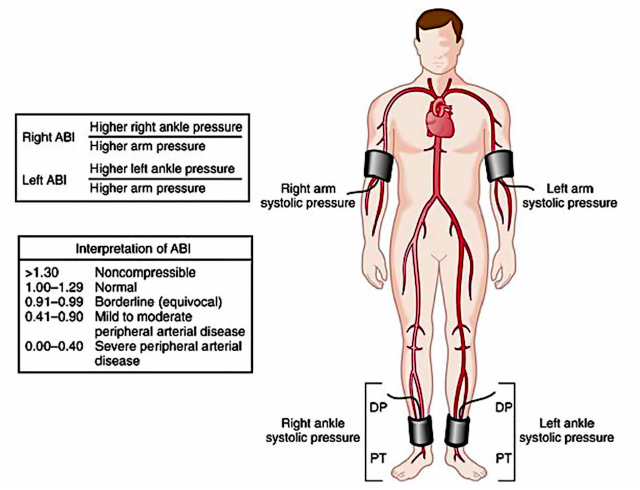
Ankle-brachial index: more than a diagnostic test?
DOI:
https://doi.org/10.47487/apcyccv.v2i4.168Keywords:
Ankle brachial index, Peripheral arterial disease, Cardiovascular risk factor, Morbidity, MortalityAbstract
The ankle-brachial index (ABI) is the relationship between the systolic blood pressure taken at the ankle level and the brachial artery. A pathological ABI (<0.90 or >1.40) indicates the presence of peripheral artery disease (PAD). Many studies indicate the great utility of this test in the diagnosis of PAD due to its ease of use, reproducibility, low cost, and high cost-effectiveness. This evaluation can be directly correlated with cardiovascular morbidity and mortality; however, it has recently been confirmed that a low ABI can be a predictor of major cardiovascular events, as it is related to diabetes mellitus, chronic coronary disease, stroke, and more. The objective of this work was to review the current evidence on the importance of ABI in the diagnosis of PAD and its main role as a predictor of cardiovascular morbidity and mortality.
Downloads
References
Aday AW, Matsushita K. Epidemiology of peripheral artery disease and polyvascular disease. Circ Res. 2021;128(12):1818-32. doi: 10.1161/CIRCRESAHA.121.318535.
Eid MA, Mehta KS, Goodney PP. Epidemiology of peripheral artery disease. Semin Vasc Surg. 2021;34(1):38-46. doi: 10.1053/j.semvascsurg.2021.02.005.
Conte MS, Bradbury AW, Kolh P, White JV, Dick F, Fitridge R, et al. Global vascular guidelines on the management of chronic limbthreatening ischemia. J Vasc Surg. 2019;69(6):3S-125S.e40. doi: 10.1016/j.jvs.2019.02.016.
Matsushita K, Ballew SH, Coresh J, Arima H, Ärnlöv J, Cirillo M, et al. Measures of chronic kidney disease and risk of incident peripheral artery disease: a collaborative meta-analysis of individual participant data. Lancet Diabetes Endocrinol. 2017;5(9):718-28. doi: 10.1016/S2213-8587(17)30183-3.
Conte MS, Bradbury AW, Kolh P, White JV, Dick F, Fitridge R, et al. Global vascular guidelines on the management of chronic limb-threatening ischemia. J Vasc Surg. 2019;69(6 Suppl):3S-125S.e40.
Dieter RS, Tomasson J, Gudjonsson T, Brown RL, Vitcenda M, Einerson J, et al. Lower extremity peripheral arterial disease in hospitalized patients with coronary artery disease. Vasc Med. 2003;8(4):233-6. doi: 10.1191/1358863x03vm506ra.
Hirsch AT, Criqui MH, Treat-Jacobson D, Regensteiner JG, Creager MA, Olin JW, et al. Peripheral Arterial Disease Detection, Awareness, and Treatment in Primary Care. JAMA. 2001;286(11):1317-24. doi: 10.1001/jama.286.11.1317.
Miguel JB, Matos JPS, Lugon JR. Ankle-Brachial Index as a Predictor of Mortality in Hemodialysis: A 5-Year Cohort Study. Arq Bras Cardiol. 2017;108(3) doi: 10.5935/abc.20170026.
Ena J, Pérez-Martín S, Argente CR, Lozano T. Association between an elevated inter-arm systolic blood pressure difference, the ankle– brachial index, and mortality in patients with diabetes mellitus. Clin Investig Arterioscler. 2020;32(3):94-100. doi: 10.1016/j.arteri.2019.11.003.
Maruhashi T, Kajikawa M, Kishimoto S, Hashimoto H, Takaeko Y, Yamaji T, et al. Upstroke Time Is a Useful Vascular Marker for Detecting Patients With Coronary Artery Disease Among Subjects With Normal Ankle‐Brachial Index. J Am Heart Assoc Cardiovasc Cerebrovasc Dis. 2020;9(23):e017139. doi: 10.1161/JAHA.120.017139.
McClary KN, Massey P. Ankle Brachial Index. En: StatPearls. Treasure Island (FL): StatPearls Publishing; 2021.
Thurston B, Dawson J. Ankle Brachial Pressure Index: An update for the vascular specialist and general practitioner. Vascular. 2019;27(5):560-70. doi: 10.1177/1708538119842395.
Lowry D, Saeed M, Narendran P, Tiwari A. A review of distribution of atherosclerosis in the lower limb arteries of patients with diabetes mellitus and peripheral vascular disease. Vasc Endovascular Surg. 2018;52(7):535-42. doi: 10.1177/1538574418791622.
Myslinski W, Stanek A, Feldo M, Mosiewicz J. Ankle-Brachial Index as the Best Predictor of First Acute Coronary Syndrome in Patients with Treated Systemic Hypertension. Biomed Res Int. 2020;2020:6471098. doi: 10.1155/2020/6471098.
Lee M-Y, Hsiao P-J, Huang J-C, Hsu W-H, Chen S-C, Chang J-M, et al. Abnormally Low or High Ankle-Brachial Index Is Associated With the Development of Diabetic Retinopathy in Type 2 Diabetes Mellitus. Sci Rep. 2018;8(1):441. doi: 10.1038/s41598-017-18882-x.
Thitiwuthikiat P, Imerbtham T, Weeraphan O, Siriwittayawan D. Improvement of Cardio-Ankle Vascular Index by Arm-Swing Exercise in Older Adults. Songklanagarind Med J. 2018;36(1):53-60.
Samba H, Guerchet M, Ndamba-Bandzouzi B, Kehoua G, Mbelesso P, Desormais I, et al. Ankle Brachial Index (ABI) predicts 2-year mortality risk among older adults in the Republic of Congo: The EPIDEMCA-FU study. Atherosclerosis. 2019;286:121-7. doi: 10.1016/j.atherosclerosis.2019.05.013.
Velescu A, Clara A, Martí R, Ramos R, Perez-Fernandez S, Marcos L, et al. Abnormally High Ankle–Brachial Index is Associated with Allcause and Cardiovascular Mortality: The REGICOR Study. Eur J Vasc Endovasc Surg. 2017;54(3):370-7. doi: 10.1016/j.ejvs.2017.06.002.
Maloberti A, Cortesi P, Micale M, Mazzaglia G, Occhi L, Palazzini M, et al. Cost-effectiveness of cardiovascular risk classification based on ankle-brachial index test in association to Framingham risk score. J Hypertens. 2021;39:e274.
Perpetuini D, Chiarelli AM, Cardone D, Rinella S, Massimino S, Bianco F, et al. Photoplethysmographic Prediction of the Ankle- Brachial Pressure Index through a Machine Learning Approach. Appl Sci. 2020;10(6):2137. doi: 10.3390/app10062137.
Penagos Cordón JC, Cifuentes Escobar LM. Utilidad diagnóstica del índice tobillo-brazo por el método palpatorio en la detección de la enfermedad arterial periférica. Rev Guatem Cardiol Impresa. 2014;24(3):2-4.
Forés R, Alzamora MT, Pera G, Torán P, Urrea M, Heras A. Concordancia entre tres métodos de medición del índice tobillobrazo para el diagnóstico de arteriopatía periférica. Med Clínica. 2014;143(8):335-40.
Alzamora MT, Forés R, Baena-Díez JM, Pera G, Toran P, Sorribes M, et al. The Peripheral Arterial disease study (PERART/ARTPER): prevalence and risk factors in the general population. BMC Public Health. 2010;10(1):38. doi: 10.1186/1471-2458-10-38.
Anand SS, Caron F, Eikelboom JW, Bosch J, Dyal L, Aboyans V, et al. Major Adverse Limb Events and Mortality in Patients With Peripheral Artery Disease. J Am Coll Cardiol. 2018;71(20):2306-15. doi: 10.1016/j.jacc.2018.03.008.
Verberk WJ, Kollias A, Stergiou GS. Automated oscillometric determination of the ankle-brachial index: a systematic review and meta-analysis. Hypertens Res Off J Jpn Soc Hypertens. 2012;35(9):883-91. doi: 10.1038/hr.2012.83.
Ichihashi S, Desormais I, Hashimoto T, Magne J, Kichikawa K, Aboyans V. Accuracy and Reliability of the Ankle Brachial Index Measurement Using a Multicuff Oscillometric Device Versus the Doppler Method. Eur J Vasc Endovasc Surg. 2020;60(3):462-8. doi: 10.1016/j.ejvs.2020.06.013.
Taneva GT, Baeza Bermejillo C, Arribas Díaz AB, González García A, Fernández Bravo J, Aparicio Martínez C. Velocidades tibiales por ecografía Doppler y validez del índice tobillo-profunda en la enfermedad arterial periférica. Angiología. 2018;70(4):163-8.
Diehm N, Shang A, Silvestro A, Do D-D, Dick F, Schmidli J, et al. Association of cardiovascular risk factors with pattern of lower limb atherosclerosis in 2659 patients undergoing angioplasty. Eur J Vasc Endovasc Surg. 2006;31(1):59-63. doi: 10.1016/j.ejvs.2005.09.006
Kodikara KG, Karunaratne WCD, Chandratilake MN. High fidelity simulation in undergraduate medical curricula: experience of fourth year medical students. South-East Asian J Med Educ. 2020;13(2):25-31.
Meijer WT, Hoes AW, Rutgers D, Bots ML, Hofman A, Grobbee DE. Peripheral arterial disease in the elderly: The Rotterdam Study. Arterioscler Thromb Vasc Biol. 1998;18(2):185-92.
Takahashi T, Tomiyama H, Aboyans V, Kumai K, Nakano H, Fujii M, et al. Association of pulse wave velocity and pressure wave reflection with the ankle-brachial pressure index in Japanese men not suffering from peripheral artery disease. Atherosclerosis. 2021;317:29-35. doi: 10.1016/j.atherosclerosis.2020.11.031.
Coyan GN, D’Angelo MP, Kilic A, Gleason TG, Luketich JD, Aranda-Michel E, et al. Evaluation of a simulation-based mini-elective on medical student interest in cardiac surgery. J Card Surg. 2019;34(10):901-7. doi: 10.1111/jocs.14143.
Criqui MH, Matsushita K, Aboyans V, Hess CN, Hicks CW, Kwan TW, et al. Lower Extremity Peripheral Artery Disease: Contemporary Epidemiology, Management Gaps, and Future Directions: A Scientific Statement From the American Heart Association. Circulation. 2021;144(9):e171-e191. doi: 10.1161/CIR.0000000000001005.
Venermo M, Sprynger M, Desormais I, Björck M, Brodmann M, Cohnert T, et al. Editor’s Choice – Follow-up of Patients After Revascularisation for Peripheral Arterial Diseases: A Consensus Document From the European Society of Cardiology Working Group on Aorta and Peripheral Vascular Diseases and the European Society for Vascular Surgery. Eur J Vasc Endovasc Surg. 2019;58(5):641-53. doi: 10.1016/j.ejvs.2019.06.017.
Recarey Pittí L del C, Mosquera Fernández A, Bellido Guerrero D. Grado de evidencia en la utilización del índice tobillo-brazo para el diagnóstico de la Arteriopatía Periférica en diabéticos tipo 2. Rev Int Cienc Podol. 2015;9(1):37-43. doi: 10.5209/rev_RICP.2015.v9.n1.47315.
Hageman D, van den Houten MML, Pesser N, Gommans LNM, Scheltinga MRM, Teijink JAW. Diagnostic accuracy of automated oscillometric determination of the ankle-brachial index in peripheral artery disease. J Vasc Surg. 2021;73(2):652-60. doi: 10.1016/j.jvs.2020.05.077.
Ruiz Comellas A, Pera G, Baena Díez JM, Heras A, Alzamora Sas MT, Forés Raurell R, et al. Relación entre actividad física en el tiempo libre y el índice tobillo-brazo en población general española: estudio ARTPER. Med Clínica. 2015;145(10):419-26.
Hiatt WR, Hess CN, Bonaca MP, Kavanagh S, Patel MR, Baumgartner I, et al. Ankle-Brachial Index for Risk Stratification in Patients With Symptomatic Peripheral Artery Disease With and Without Prior Lower Extremity Revascularization: Observations From the EUCLID Trial. Circ Cardiovasc Interv. 2021;14(7):e009871. doi: 10.1161/CIRCINTERVENTIONS.120.009871.
Diehm N, Shang A, Silvestro A, Do D-D, Dick F, Schmidli J, et al. Association of cardiovascular risk factors with pattern of lower limb atherosclerosis in 2659 patients undergoing angioplasty. Eur J Vasc Endovasc Surg. 2006;31(1):59-63. doi: 10.1016/j.ejvs.2005.09.006.
Kärberg K, Lember M. Subclinical atherosclerosis in the carotid artery: can the ankle-brachial index predict it in type 2 diabetes patients? Scand J Clin Lab Invest. 2021;81(3):237-43. doi: 10.1080/00365513.2021.1904279.
Oliveras V, Martín-Baranera M, Gracia M, del Val JL, Plans M, Pujol-Moix N. Importancia del índice tobillo-brazo en la reclasificación del riesgo cardiovascular de varones hipertensos asintomáticos de mediana edad. Med Clínica. 2015;144(10):435-9.
Ramos MV, Ramos MV. Aspectos destacados de las Guías de la Sociedad Europea de Cardiología sobre cardiología deportiva y ejercicio en pacientes con enfermedad cardiovascular. Rev Urug Cardiol. 2020;35(3):61-86.
Abdelmonaem M, Reda A, Nour A. Correlation Between Ankle Brachial Index and SYNTAX Score to Predict Severity of Coronary Artery Disease [Internet]. Vascular Disease Management. 2021 [citado 12 de septiembre de 2021]. Disponible en: https://www.hmpgloballearningnetwork.com/site/vdm/content/correlationbetween-ankle-brachial-index-and-syntax-score-predict-severitycoronary-artery
Sharma AK, Kejriwal MP, Sinha SK, Razi M M, Pandey U, Shukla P, Thakur R, Verma C M, Krishna V. A comparative assessment of the severity of coronary artery disease in patients with low ankle–Brachial index and normal ankle–Brachial index: An angiographybased cross-sectional observational-analytical study (CADLABI study). J Pract Cardiovasc Sci 2021;7:54-9.
Núñez D, Morillas P, Quiles J, Cordero A, Guindo J, Soria F, et al. Utilidad de un índice tobillo-brazo patológico en la identificación de la enfermedad coronaria multivaso en pacientes con síndrome coronario agudo. Rev Esp Cardiol. 2010;63(1):54-9.
Pichín Quesada A, Goulet Ordaz L, Suárez Lescay C, Franco Mora M del C. Pacientes con cardiopatía isquémica y enfermedad arterial periférica asintomática determinada mediante el índice tobillo-brazo. MEDISAN. 2017;21(1):1-11.
Strandness D, Priest R, Gibbons G. Combined clinical and pathologic study of diabetic and nondiabetic peripheral arterial disease. Diabetes. 1964;13(4):366-72.
Garduño LMM, Rocha RB, Pérez FJG, Salinas CAA. Relación del índice tobillo/brazo determinado por ultrasonido Doppler con desenlaces cardiovasculares y amputación en un grupo de pacientes con diabetes mellitus 2 estudiados en el Instituto Nacional de Ciencias Médicas y Nutrición Salvador Zubirán. Gac Med Mex. 2011;147(2):111-6.
Domínguez GV, Cabrera HM. Evaluación de la concordancia entre los valores del índice tobillo-brazo y presiones segmentarias con amputacion del pie diabético. Rev Soc Peru Med Interna. 2013;26(4):184-92.
Baghdasaryan PA, Bae JH, Yu W, Rowe V, Armstrong DG, Shavelle DM, et al. “The Renal Foot”-Angiographic Pattern of Patients with Chronic Limb Threatening Ischemia and End-Stage Renal Disease. Cardiovasc Revasc Med. 2020;21(1):118-21. doi: 10.1016/j.carrev.2019.09.001.
Garimella PS, Hirsch AT. Peripheral Artery Disease and Chronic Kidney Disease: Clinical Synergy to Improve Outcomes. Adv Chronic Kidney Dis. 2014;21(6):460-71. doi: 10.1053/j.ackd.2014.07.005.
Chen H-Y, Wei F, Wang L-H, Wang Z, Meng J, Yu H-B, et al. Abnormal ankle-brachial index and risk of cardiovascular or all-cause mortality in patients with chronic kidney disease: a meta-analysis. J Nephrol. 2017;30(4):493-501. doi: 10.1007/s40620-017-0376-z.
Ratnatunga P, Gunawardene R, Pinto V, Perera R, Amerasinghe P, Hewavithana P, et al. Atherosclerotic occlusive arterial disease of the lower limbs: a historical account of surgical evolution and vascular reconstruction over thirty four years. Sri Lanka J Surg. 2018;36(2):1-7. doi: 10.4038/sljs.v36i2.8508.
Fuglestad MA, Hernandez H, Gao Y, Ybay H, Schieber MN, Brunette KE, et al. A low-cost, wireless near-infrared spectroscopy device detects the presence of lower extremity atherosclerosis as measured by computed tomographic angiography and characterizes walking impairment in peripheral artery disease. J Vasc Surg. 2020;71(3):946-57. doi: 10.1016/j.jvs.2019.04.493.
Oriol Torón PÁ, Badía Farré T, Romaguera Lliso A, Roda Diestro J. Síndrome metabólico y enfermedad arterial periférica: 2 enfermedades relacionadas. Endocrinol Nutr. 2016;63(6):258-64.
Estirado E, Lahoz C, Laguna F, García-Iglesias F, González-Alegre MT, Mostaza JM. Síndrome metabólico en pacientes con enfermedad arterial periférica. Rev Clínica Esp. 2014;214(8):437-44.
Hong JB, Leonards CO, Endres M, Siegerink B, Liman TG. Ankle-Brachial Index and Recurrent Stroke Risk: Meta-Analysis. Stroke. 2016;47(2):317-22. doi: 10.1161/STROKEAHA.115.011321.
Sander D, Poppert H, Sander K, Etgen T. The role of intima-mediathickness, ankle-brachial-index and inflammatory biochemical parameters for stroke risk prediction: a systematic review. Eur J Neurol. 2012;19(4):544-e36. doi: 10.1111/j.1468-1331.2011.03510.x.
Fan H, Hu X, Yu W, Cao H, Wang J, Li J, et al. Low ankle-brachial index and risk of stroke. Atherosclerosis. 2013;229(2):317-23. doi: 10.1016/j.atherosclerosis.2013.05.014.